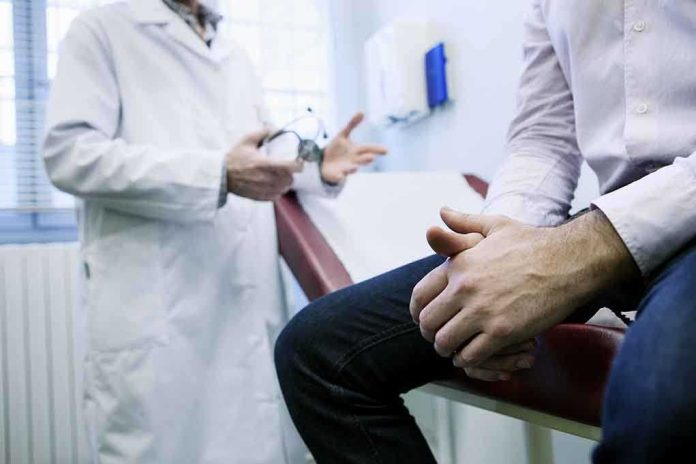
A trusted Ohio physician just received a 64-month prison sentence for rubber-stamping $14.5 million in fraudulent Medicare claims without ever examining a single patient he claimed to treat.
Story Snapshot
- Dr. Timothy Sutton sentenced to over 5 years in prison for massive Medicare fraud scheme
- Approved pre-completed medical orders for braces and genetic tests without patient contact
- Ordered to pay nearly $6 million in restitution to federal health programs
- Case highlights growing federal crackdown on telemedicine fraud abuse
The Digital Deception That Fooled Medicare
Timothy Sutton operated what federal investigators called a “paper mill” medical practice from his North Ridgeville office. The 44-year-old physician worked for unnamed Florida-based telemedicine companies, digitally signing medical orders that arrived pre-completed on his desk. Each signature falsely certified that he had examined patients and determined their medical needs for expensive durable medical equipment and cancer genetic testing.
Ohio Physician Gets 5 Years in Prison for Role in $14.5M Medicare Fraud
https://t.co/IkpkBaWppn— Townhall Updates (@TownhallUpdates) January 18, 2026
U.S. District Judge David A. Ruiz imposed the 64-month sentence on January 12, 2026, after Sutton pleaded guilty to conspiracy to commit wire and mail fraud, making false healthcare statements, and aggravated identity theft. The scheme defrauded Medicare of over $14.5 million in false claims, though Sutton will pay back only $6 million in restitution.
A Physician’s Oath Becomes a Criminal Enterprise
Federal prosecutors revealed that Sutton never conducted telemedicine examinations despite claiming to be the treating physician for hundreds of patients. His role involved approving orders for medical braces and cancer genetic screenings that were then sold to other entities within the conspiracy network. The orders flowed through multiple companies, creating layers of separation between the fraudulent approvals and the final billing to Medicare.
U.S. Attorney David M. Toepfer emphasized the betrayal of public trust, stating that Sutton “deliberately lied about examining patients via telemedicine and fraudulently affirmed that he was the treating physician.” This systematic deception allowed unscrupulous companies to extract millions from taxpayer-funded healthcare programs designed to help legitimate patients.
Federal Enforcement Sends Clear Warning
The Sutton case represents a broader Justice Department initiative targeting telemedicine fraud that exploded during the COVID-19 pandemic. The FBI Cleveland Division and Health and Human Services Office of Inspector General conducted the investigation, uncovering a pattern of abuse that extends far beyond one rogue physician.
FBI Special Agent in Charge Gregory Nelsen characterized the fraud as “cruel and calculating,” noting that such schemes force taxpayers to subsidize unnecessary medical equipment while legitimate patients face higher costs and reduced access to care. HHS-OIG Special Agent Mario M. Pinto added that physician participation in fraud “erodes trust in our health care system” when doctors violate their fundamental oath to do no harm.
The Price of Medical License Abuse
Sutton will serve three years of supervised release following his prison term, during which time federal probation officers will monitor his activities and finances. The case demonstrates how quickly legitimate medical credentials can become criminal tools when physicians prioritize easy money over patient welfare and professional ethics.
This sentencing occurs as the Justice Department has established a new Enforcement and Affirmative Litigation branch specifically targeting healthcare fraud, including telemedicine schemes, medical necessity disputes, and systematic billing abuse. The message to healthcare providers is unmistakable: federal agencies now possess sophisticated tools to detect fraudulent patterns and will pursue maximum penalties for those who exploit vulnerable patients and taxpayer-funded programs.
Sources:
Ohio Physician Gets 64 Months for Role in $14.5M Medicare Fraud
DOJ rolls out new healthcare fraud unit: 5 things to know




